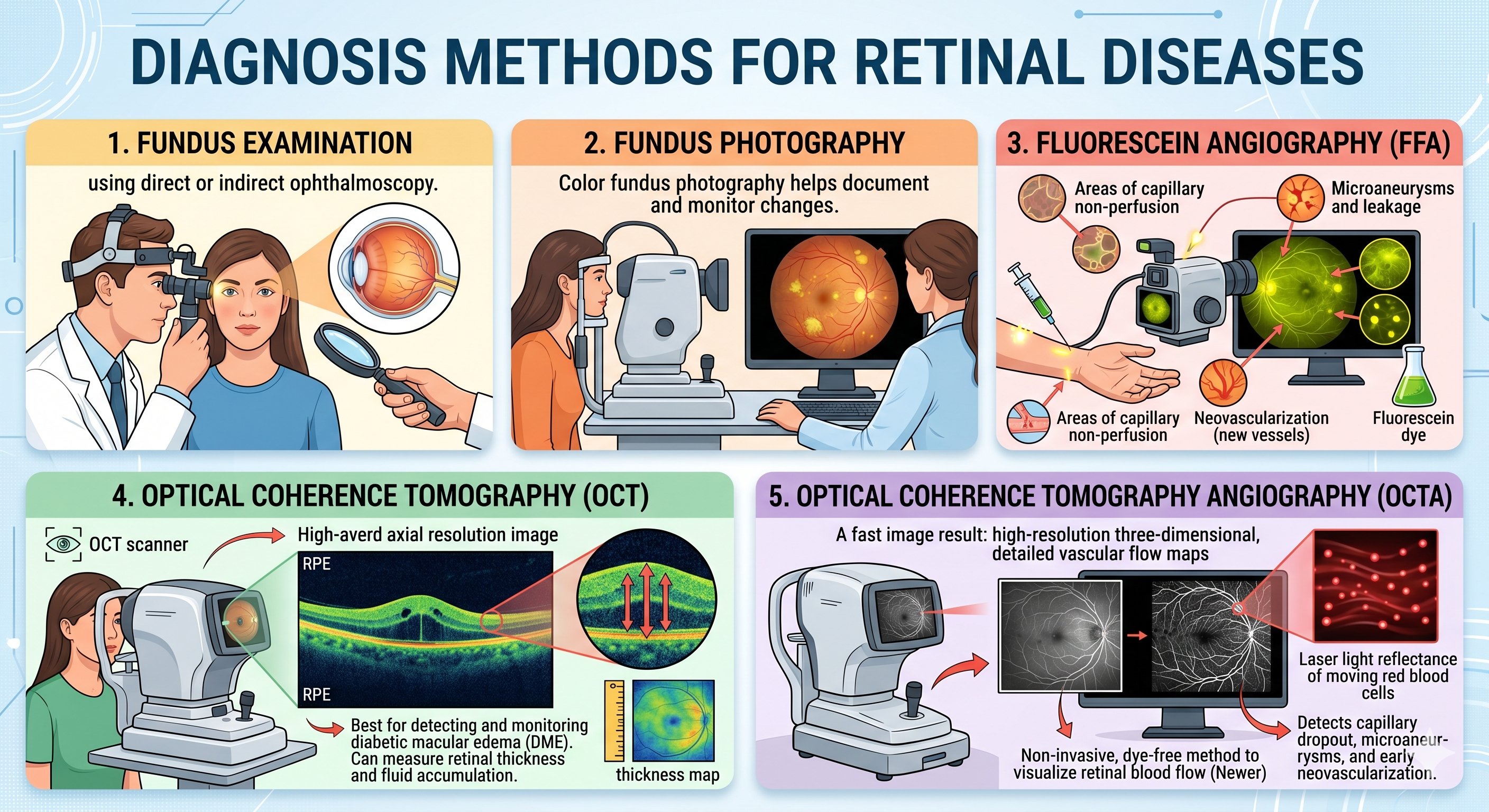
Diagnosis methods
Fundus examination using direct or indirect ophthalmoscopy
- Fundus Photography
o Color fundus photography helps document and monitor changes.
- Fluorescein Angiography (FFA)
o Inject fluorescein dye and take retinal images.
oIdentifies: Areas of capillary non-perfusion, Neovascularization, Microaneurysms and leakage
- Optical Coherence Tomography (OCT)
o Cross-sectional imaging of the retina.
o Best for detecting and monitoring diabetic macular edema (DME).
o Can measure retinal thickness and fluid accumulation.
- Optical Coherence Tomography Angiography (OCTA) (Newer)
o Non-invasive, dye-free method to visualize retinal blood flow.
o Laser light reflectance of the surface of moving red blood cells to accurately depict vessels
o Detects capillary dropout, microaneurysms, and early neovascularization.
Management
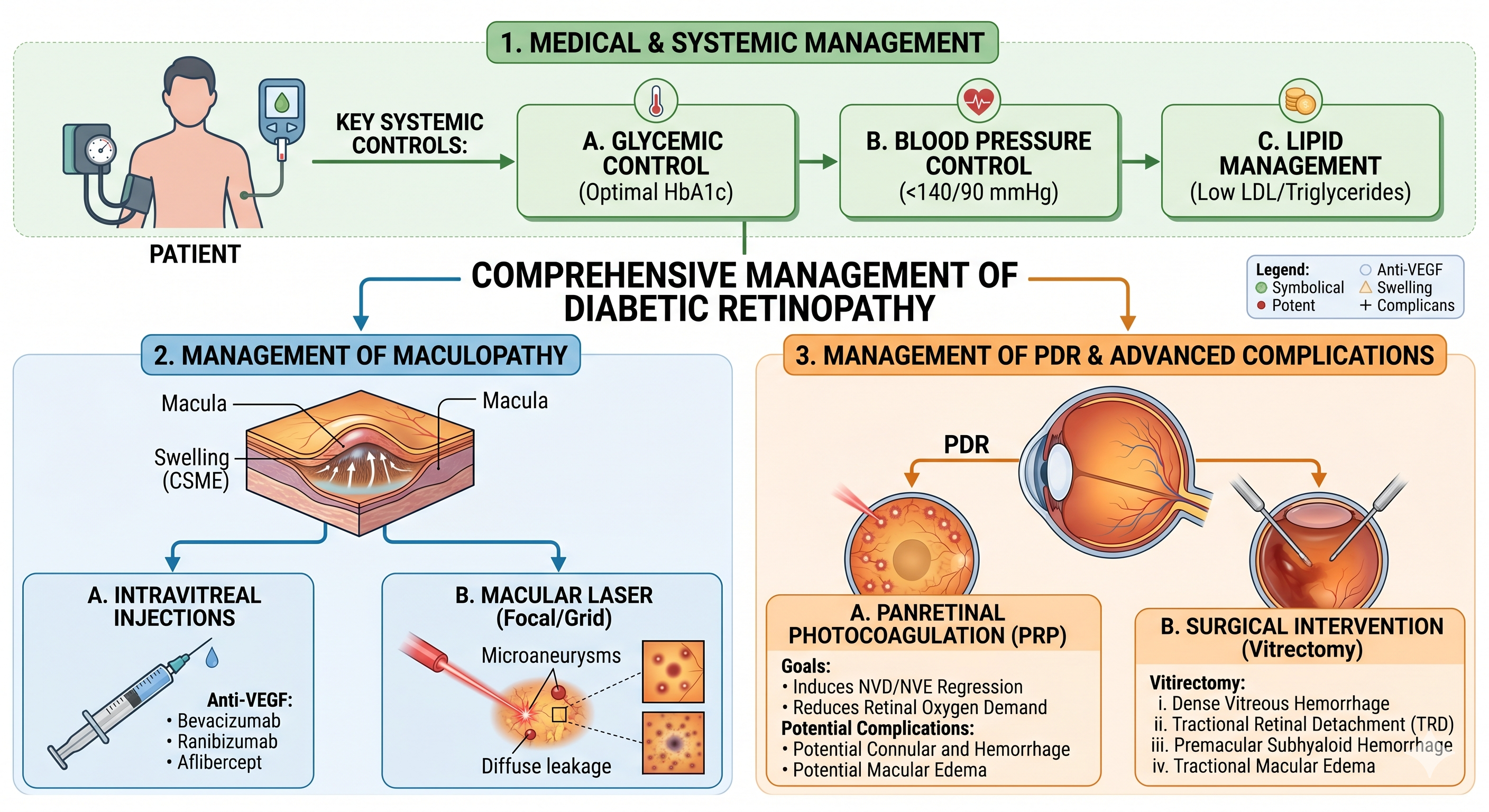
The management of diabetic retinopathy is categorized by the severity of the disease and the presence of specific complications like macular edema.
Medical and Systemic Management
Effective management begins with controlling the underlying systemic factors that drive retinal damage:
- Glycemic Control: Maintaining optimal blood glucose levels is essential to slow the progression of retinopathy.
- Blood Pressure Control: Strict management of systemic hypertension reduces the risk of retinal hemorrhages and edema.
- Lipid Management: Control of serum lipids is particularly important in managing hard exudates and maculopathy.
Management of Diabetic Maculopathy
Treatment for maculopathy is indicated when there is clinically significant macular edema (CSME)
- Laser Photocoagulation
- Focal treatment: Targeted at specific leaking microaneurysms or areas of capillary leakage.
- Grid treatment: Applied to areas of diffuse capillary leakage or retinal thickening
- Pharmacotherapy: Intravitreal injections of Anti-VEGF (Vascular Endothelial Growth Factor) agents or steroids may be used to reduce macular thickening
Management of Proliferative Diabetic Retinopathy (PDR)
The goal of treating PDR is to induce regression of neovascularization.
- Panretinal Photocoagulation (PRP):
- This is the standard treatment for PDR.
- Laser burns are applied to the peripheral retina, sparing the macula.
- The objective is to reduce the overall oxygen demand of the retina, which leads to the regression of new vessels.
- Complications of PRP can include reduced peripheral vision and impaired night vision
Surgical Management (Vitrectomy)
Pars plana vitrectomy is indicated for advanced complications of diabetic retinopathy.
- Vitreous Hemorrhage: Persistent hemorrhage that fails to clear and prevents laser treatment.
- Tractional Retinal Detachment : Specifically when involving or threatening the macula.
- Combined Tractional and Rhegmatogenous Retinal Detachment
- Premacular Subhyaloid Hemorrhage
- Persistent Macular Edema In cases with associated posterior hyaloid traction.