Classification of diabetic retinopathy
Diabetic retinopathy is classified into two primary stages: non-proliferative diabetic retinopathy (NPDR) and proliferative diabetic retinopathy (PDR).
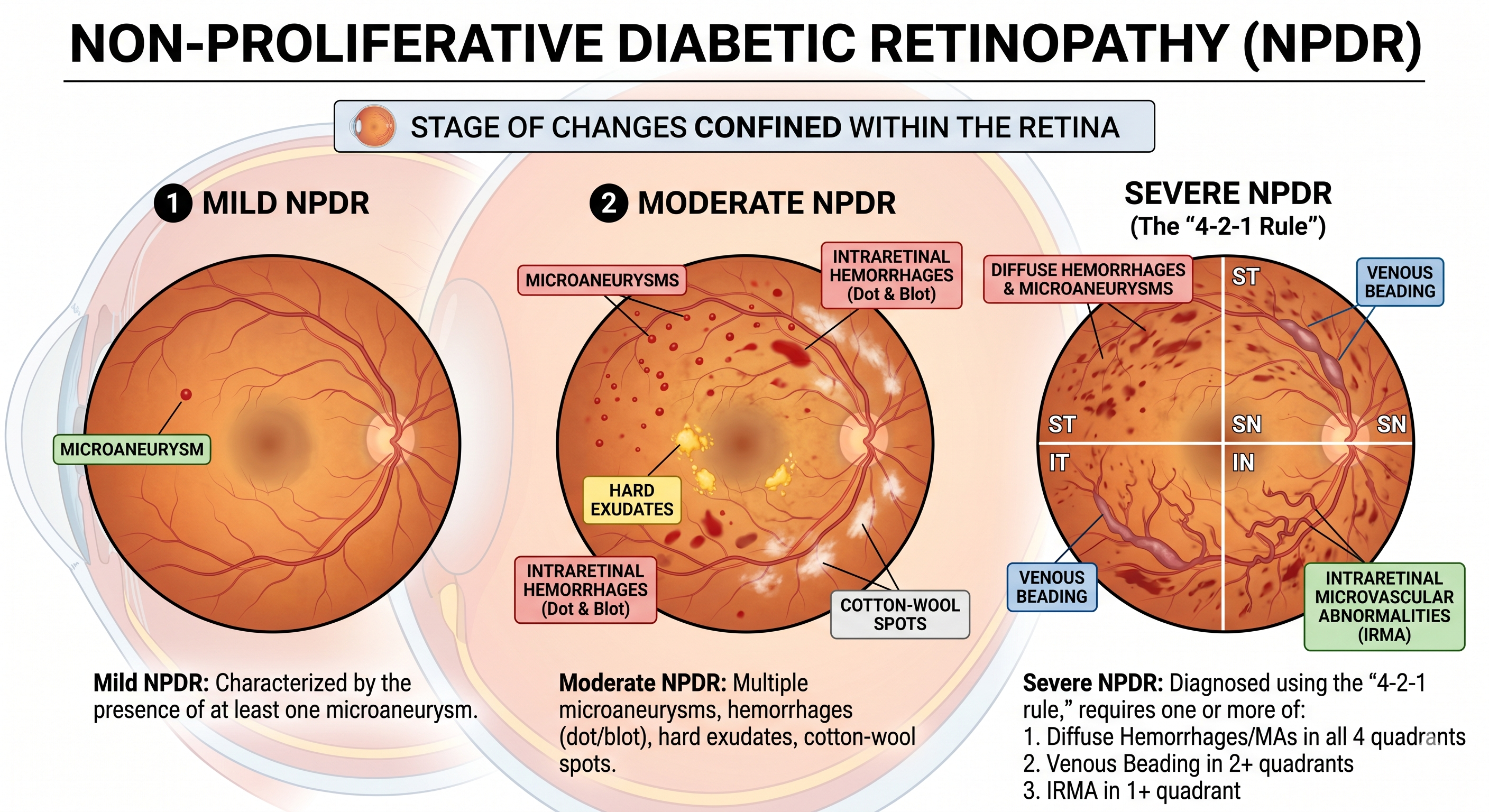
This stage is characterized by changes confined within the retina and is further subdivided based on severity:
- Mild NPDR: Characterized by the presence of at least one microaneurysm.
- Moderate NPDR: Features multiple microaneurysms, intraretinal hemorrhages (dot and blot), hard exudates, and cotton-wool spots.
- Severe NPDR: Diagnosed using the “4-2-1 rule,” which requires the presence of one or more of the following:
- Diffuse intraretinal haemorrhages and microaneurysms in all four quadrants.
- Venous beading in two or more quadrants.
- Intraretinal microvascular abnormalities (IRMA) in at least one quadrant.
Proliferative Diabetic Retinopathy (PDR)
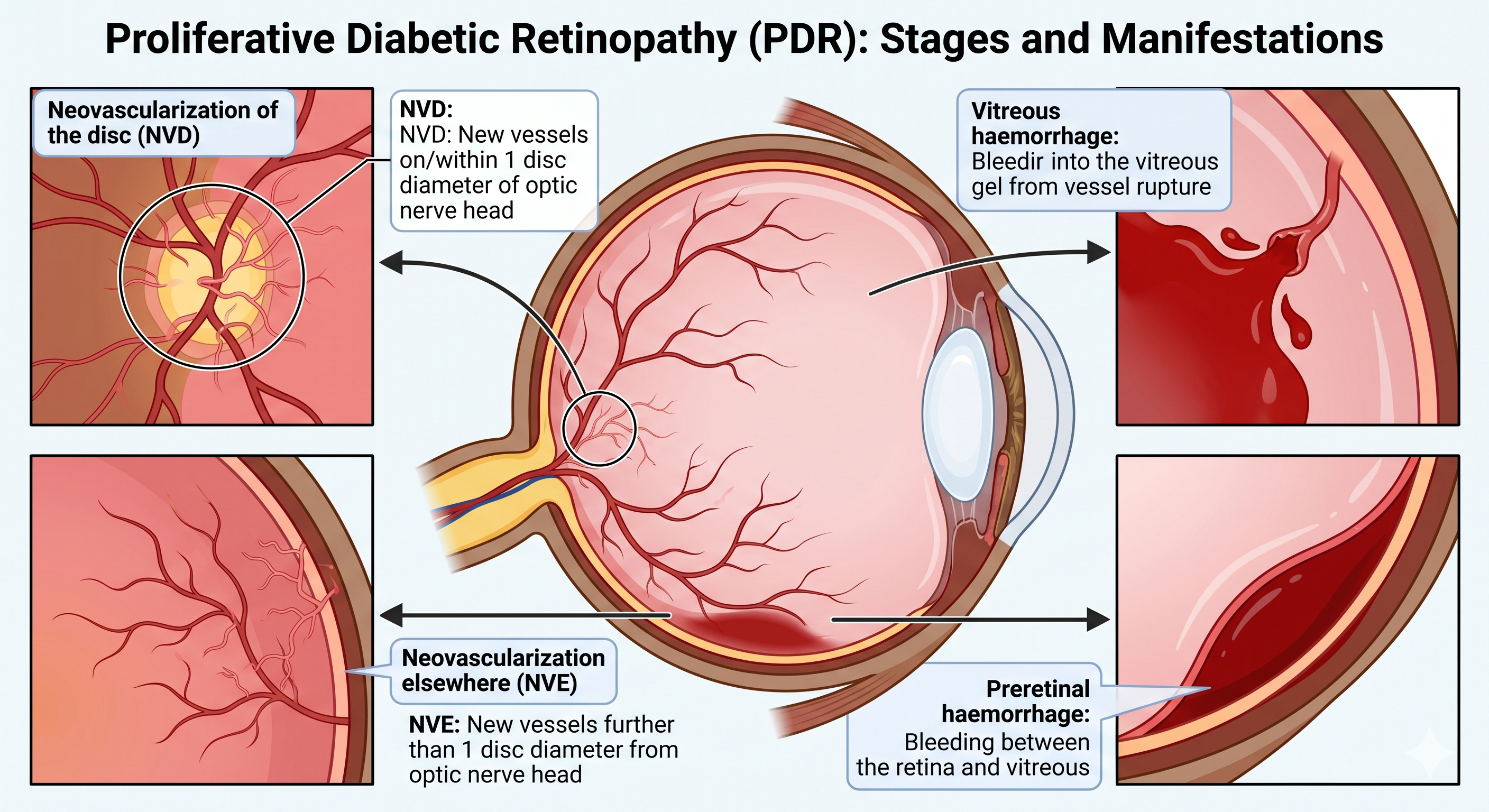
This stage is defined by the presence of neovascularization, which is the growth of new, fragile blood vessels:
- Neovascularization of the disc (NVD): New vessels located on or within one disc diameter of the optic nerve head.
- Neovascularization elsewhere (NVE): New vessels located further than one disc diameter from the optic nerve head.
- Vitreous haemorrhage: Bleeding into the vitreous gel resulting from the rupture of these new vessels.
- Preretinal haemorrhage: Bleeding between the retina and the vitreous.
Diabetic Maculopathy
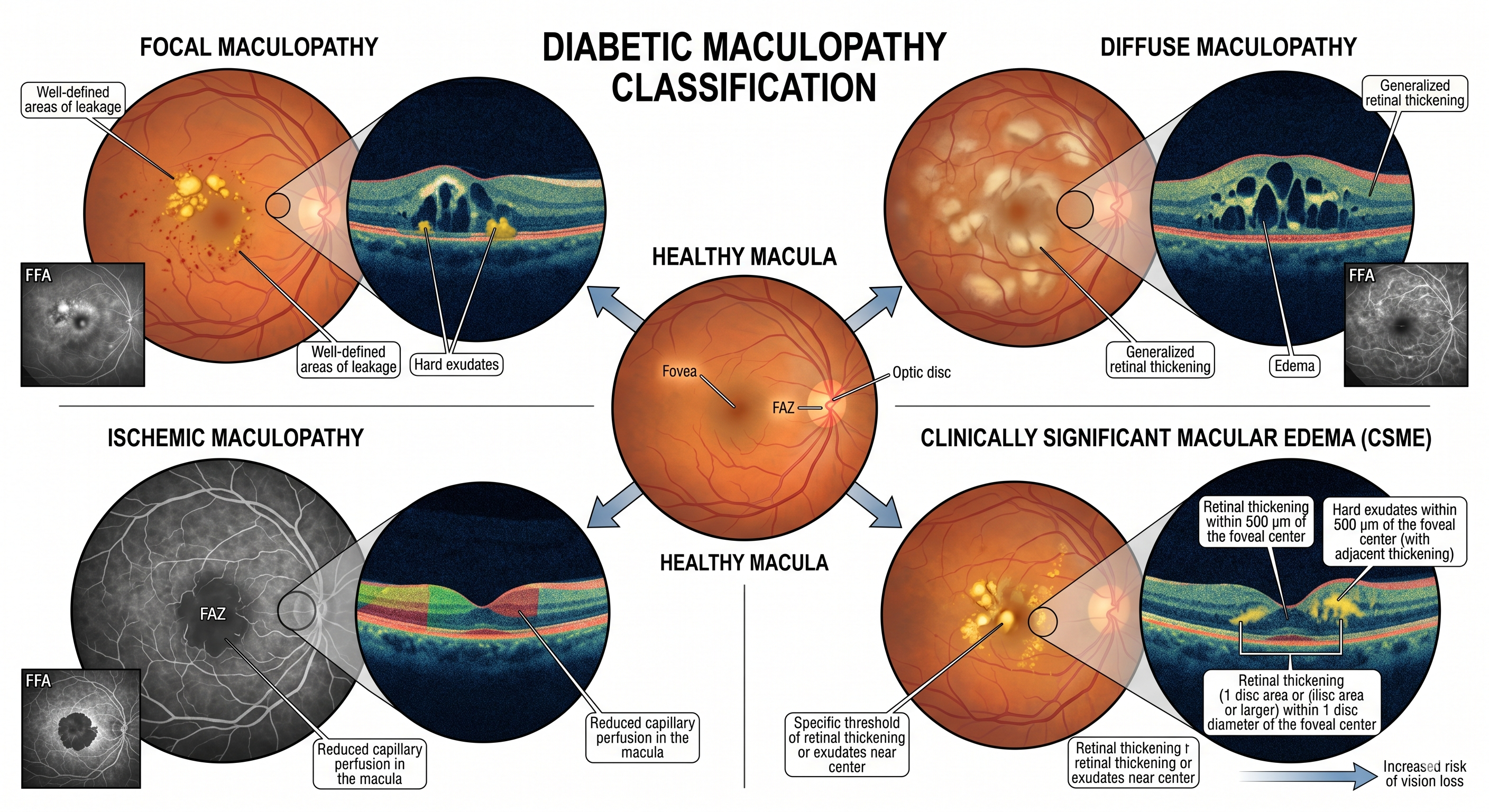
This classification can occur at any stage of diabetic retinopathy and specifically involves the macula:
- Focal Maculopathy: Well-defined areas of leakage and hard exudates.
- Diffuse Maculopathy: Generalized retinal thickening and edema.
- Ischemic Maculopathy: Reduced capillary perfusion in the macula.
- Clinically Significant Macular Edema (CSME): A specific threshold of retinal thickening or exudates near the centre of the macula that increases the risk of vision loss.